

Part I: The Issue
Beginning in the 1960s, with the rising concern about non-marital adolescent pregnancy and the pandemic of HIV/AIDS after 1981, sex education became critically important public health and policy issue in the United States (Hall et al. 595). The need for and acceptance of formal instruction for adolescents on life-saving topics such as contraception, condoms, and sexually transmitted infections, became widely implemented in school and community-based programs in the late 1980s and early 1990s (Hall et al. 595). However, in the late 1990s, as part of the “welfare reform,” abstinence-only until marriage sex education was adopted by the U.S. government as a singular approach to adolescent sexual and reproductive health (Hall et al. 595). Abstinence only until marriage (AOUM) sex education received a variety of funding from domestic and foreign aid programs, leading 49 of 50 states accepting federal funds to promote it in the classroom (Hall et al. 595).
Since then, research has proven AOUM sex education as ineffective. It lacks efficacy in delaying sexual initiation, reducing sexual risk behavior or improving reproductive health outcomes. Additionally, it does not increase condom and contraceptive use or contribute to decreased pregnancy rates among adolescents (Hall et al. 595). According to the researchers, AOUM programs also violate adolescent human rights, withhold medically accurate information, stigmatize or exclude many youth, reinforce harmful gender stereotypes, and undermine public health programs. Between 2002 and 2014, the percentage of schools in the U.S. that require students to learn about human sexuality fell from 67 percent to 48 percent, and requirements for HIV prevention declined from 64 to 41 percent. In 1995, 81 percent of adolescent males and 87 percent of adolescent females reported receiving formal instruction about birth control methods compared to only 55 and 60 percent said the same by 2011-2013.
Even though abstinence only until marriage sex education programs are widely rejected by health professionals, including the Society for Adolescent Health and Medicine, Congress has spent over $2 billion on domestic abstinence-only programs between 1982 and 2017. Data from 2017 reveals that funding towards these programs totals $85 million per year. Because of these guidelines, U.S. states cannot use funds to educate adolescent about contraceptive use or discuss contraceptive methods, except to emphasize failure rates.
At the state level, individual states, districts, and school boards determine implementation of federal policies and funds (Hall et al. 595). Limited in-class time and resources leave school to prioritize sex education in competition with academic subjects and other important health topics such as substance use, bullying, and suicide (Hall et al. 595). Nevertheless, nearly all students receive some sort of sex education. Therefore, the problem is not whether students receive sex education, but rather its quality.
Sex education, particularly regarding issues of abstinence and gender, varies widely between states. Only 13 of 50 states require sex education to be medically accurate. Nineteen out of fifty states have information on contraception included in their sex education programs, and legislation in half of the states stresses abstinence. That being said, most of U.S. public school students do not receive instruction through their state’s sex education program on how to identify healthy and unhealthy relationship behaviors.
One of the states in which sex education is not mandated is Louisiana. Still, schools must teach health education, which includes instruction on sexual risk behaviors, HIV/AIDS, and other STDs. In schools where sex education is offered, curriculum must emphasize abstinence as the expected social standard. Additionally, curriculum is not required to include instruction on consent or any sexually explicit materials depicting homosexual activity. They also may not in any way counsel or advocate abortion. Classes emphasize that abstinence from sexual activity outside of marriage is the expected standard for all school-age children and it is a way to avoid unwanted pregnancy, STDs, including AIDS, and other associated health problems. Louisiana also has no standard regarding medically accurate sex education instruction. When school chooses to teach sex education, instruction must be based on factual biological or pathological information.
Centers for Disease Control and Prevention released the School Health Profiles, which measure school health policies and practices and highlight which health topics were taught in schools. In the School Health Profiles, which were updated in 2019, the CDC identifies 20 sexual health education topics as critical for ensuring a young person’s sexual health. Louisiana’s last time in the School Health Profiles was for the 2015-2016 year when the CDC identified only 19 sexual health education topics. Only 11% of Louisiana schools taught students all critical sexual health education topics in a required course for grades 6-8. For grades 9-12, sixteen percent of Louisiana secondary schools taught students all of the topics.
The Louisiana Adolescent Reproductive Health Coalition (LARHC), formed in 2015, tried to advance sex education at the local level. Unfortunately, LARHC has had limited success in districts including New Orleans, as the Orleans Parish School Board dissolved in 2005 following Hurricane Katrina. Because of that, New Orleans schools are entirely handled by charter management organizations (CMOs) whose policies can allow for better sex education in some schools, but not all of them. This inconsistency between schools only contributes to other inequities. Such discrepancies provides result in policies and curricula that stigmatize marginalized youth, such as students of color and LGBTQ youth. It presents further challenges in ensuring that low-income districts have access to the resources needed to implement better sex education. To continue to advance sex education, advocates note that a culture of accountability and evaluation of learning standards is necessary for new, comprehensive policy implementation.
Part II: The Solution
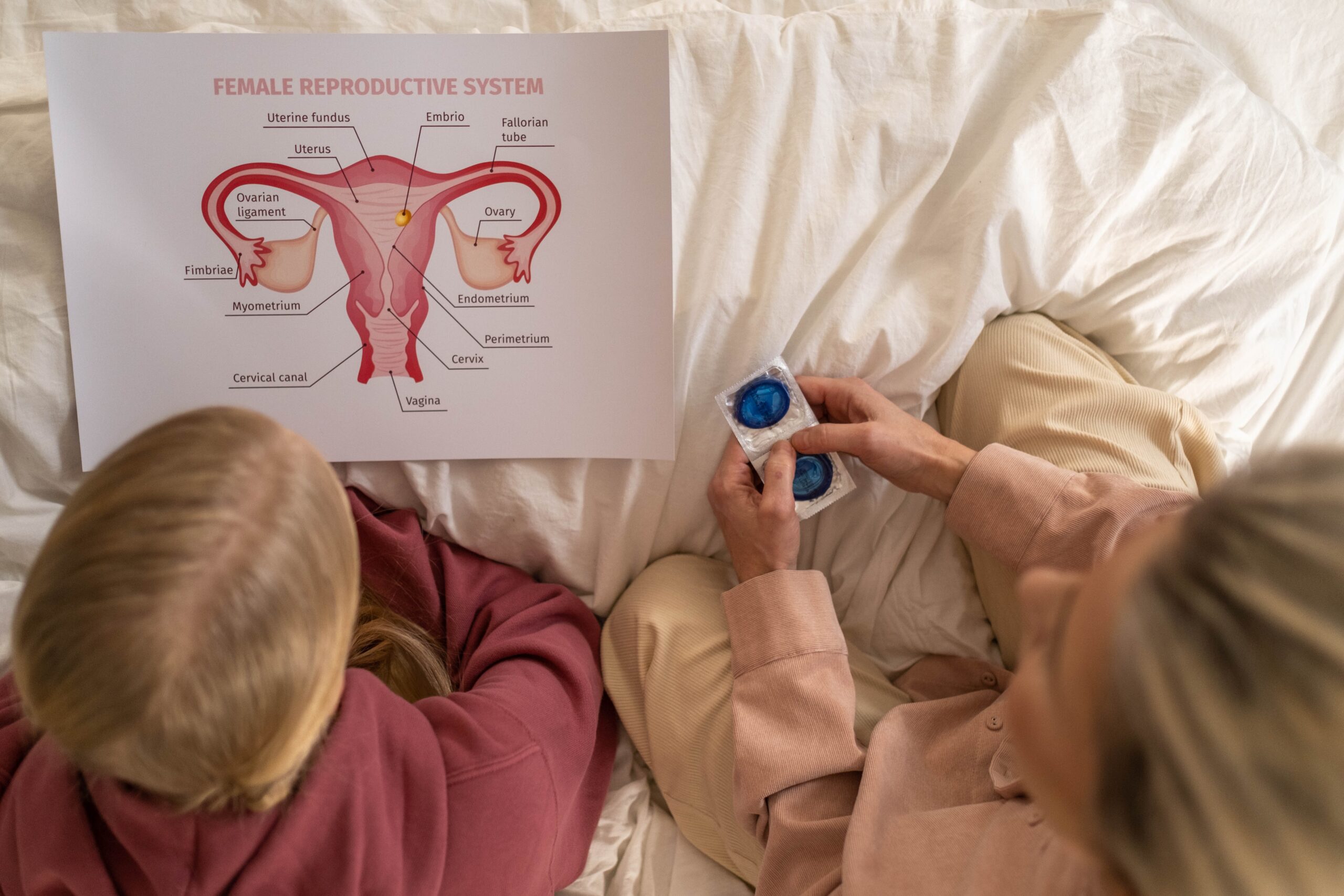
An adolescent being taught about sexual education (Photo by cottonbro, Pexels)
Even though the United States are slowly recognizing the insufficient state of sex education, effort to implementing more ambiguous, forward-thinking strategies that cross-cut levels to translate and expanded evidence into best practices and policies should be made (Hall et al. 596). Compared to abstinence-only programs, comprehensive sex education programs have favorable effects on adolescent behaviors. This includes sexual initiation, number of sex partners, frequency of sexual activity, use of condoms and contraception, frequency of unprotected sexual activity, STIs, and pregnancy.
According to the Sexuality Information and Education Council of the United States, comprehensive sex education programs include “developmentally and culturally responsive, science-based and medically accurate information on a broad set of topics related to sexuality, including human development, relationships, personal skills, sexual health and society and culture.” Comprehensive sex education focuses on a student as a whole, including the emotional, psychosocial and economic impacts of what happens when youth and adolescents engage in sexual intercourse and other sexual practices.
One state that was successful in implementing progressive sex and gender education curriculum in public schools was California. The significant success in advancing sex education in California is largely due to the passage of the California Healthy Youth Act (CHYA) in 2015 and an equivalent version for charter schools that passed in 2018. CHYA requires school districts to provide comprehensive sex education. Sex or HIV education in California must be medically accurate, age and culturally appropriate, unbiased, and cannot promote religion. It must include contraception and cover, rather than stress abstinence. Importance of sex only within marriage and negative outcomes of teen sex must not be included or discussed. Additionally, sex education must be inclusive of sexual orientation. It also must include life skills on sexual consent, healthy relationships, sexual decision-making and self-discipline. Lastly, it provides life skills on dating and sexual violence prevention.
Advocates report that districts in California often use Be.Real. Be.Ready, Making Proud Choices!, Positive Prevention Plus, Rights, Respect, Responsibility (3R’s), and Teen Talk/Puberty Talk to provide students with comprehensive instruction. The Health Education Curriculum Framework has also been recently updated to provide guidance for educators that teach sex education. The curriculum includes the use of inclusive language and instruction on consent. In 2018, legislation allowed schools to provide instruction on the potential risks of sharing sexually suggestive or explicit materials through digital media. Additionally, it requires schools to include information on how social media and mobile devices are used for human trafficking.
However, even though California is one of the states whose comprehensive sex education has been used as a model to advance sex education nationwide, California’s own rural and low-income communities continue to lack support in implementing comprehensive curriculum. To assist with the continued implementation of the CHYA, several coordinated efforts across California are underway to ensure youth are receiving comprehensive sex education.
The Sexual Health Education Roundtable, made up of a variety of California educators, researchers, health providers, and advocates, have worked since 2002 to strengthen sex education through legislation, funding, and administrative guidance. Organizations such as California Latinas for Reproductive Justice advocate for comprehensive sex education and address misinformation spread about the CHYA through community education efforts. The Adolescent Sexual Health Work Group is also dedicated to the continued promotion and protection of legislation concerning youth sexual and reproductive health in California. Districts, such as the San Diego Unified School District, guide the state to support the implementation of a curriculum that aligns with the CHYA. Advocates are also working to address gaps in the curriculum requirements, including the need for more explicit provisions in grades six and K-5, as current conditions have been described as “ambiguous” and sparked controversy.
North Carolina schools also took a step towards providing students with more comprehensive sex education. They started implementing Teen Prevention Education Program (TPP) as a promising strategy to reduce teen pregnancy and related risk behaviors (Layzer et al. S71). The Teen PEP program, which was developed in New Jersey by the Center for Supportive Schools and HiTOPS Adolescent Health and Education Center, provides a model for school-based comprehensive sexual health education both for its use of peer education and for the activity-based learning approach used to convey information (Layzer et al. S70). Implementation of Teen PEP occurs by assembling and training a team of stakeholders and program advisors and recruiting, selecting, and training a group of 11th- and 12th-grade peer educators (Layzer et al. S71). The program is then integrated into the school day; it leverages existing resources within the school (staff, students, and space), delivers comprehensive training to program advisors and student peer educators, and includes a broad sexual health focus (Layzer et al. S71). The majority of participants reported that Teen PEP had helped them learn about sexual health topics that have not previously been addressed in their educational experience. Additionally, they said greater familiarity with community resources, increased feelings of connectedness to school, and perceived cognitive and behavioral changes that could transfer to preventing other risky behaviors (Layzer et al. S77).
Part III: Implementation
Changing legislation as a whole would be an ideal solution for the state of Louisiana as well as city of New Orleans. However, it is hard to get legislators behind comprehensive sex education, because controversial and sensitive topics such as sexual orientation and contraception, which are unaddressed in many states, make lawmakers uncomfortable. It can take years to transform disjointed sex education laws into comprehensive requirements that lead to better health outcomes for adolescents in public schools, because legislation is part of a nationwide trend. The instruction about sex education is therefore often left to underfunded non-profit groups. Mandated, federally funded comprehensive sex education should include people with diverse sexual orientations, gender identities, socioeconomic backgrounds, levels of pre-existing health literacy, and ethnic and cultural backgrounds. As one of the most varied places in the U.S., New Orleans offers an excellent place for people with diverse backgrounds to gather and promote comprehensive sex education.
First, legislators should educate themselves on the issue of not providing students with comprehensive sex education. School districts of New Orleans should educate their teachers on the importance and positive outcomes of comprehensive sex education. It is hard to demand from teachers to have knowledge of or ability to teach comprehensive sex education instead of teaching all other subjects. This is where legislators could use the help of community partners.
Community partners and non-profit organizations like Planned Parenthood and Advocates for Youth are themselves offering comprehensive sex education. Planned Parenthood’s Teen Peer-Led Sex Ed initiatives spread knowledge and know-how that peers in schools can extend. New Orleans, as a place that still refuses to disseminate this sometimes life-saving information, can be an excellent place for these organizations to intertwine. In these programs, young people are encouraged to educate one another and their community about safe and healthy relationships. School districts could provide time for these organizations to come into schools and educate youth about developmentally and culturally responsive, science-based, and medically accurate information on a broad set of topics related to sexuality, including human development, relationships, personal skills, and sexual health, and society and culture.
School districts of New Orleans should also update their sex education curriculum to include information for teachers on how to tackle these important topics. To do that, advocates could use the information that has been proven successful in California. Including sources such as Be.Real. Be. Ready, Making Proud Choices!, Positive Prevention Plus, Rights, Respect, Responsibility (3R’s), and Teen Talk/Puberty Talk, which have been proven effective, into the curriculum, would equip teachers to provide students with comprehensive instruction. Implementing these small but powerful changes into the curriculum would make teachers aware of the importance of comprehensive sex education and allow students to be adequately educated on the topic.
Works Cited
Hall, Kelli Stidham, et al. “The State of Sex Education in the United States.” Journal of Adolescent Health, vol. 58, no. 6, Elsevier Inc, 2016, pp. 595–97, https://doi.org/10.1016/j.jadohealth.2016.03.032.
Layzer, Carolyn, et al. “A Peer Education Program: Delivering Highly Reliable Sexual Health Promotion Messages in Schools.” Journal of Adolescent Health, vol. 54, no. 3, Elsevier Inc, 2014, pp. S70–S77, https://doi.org/10.1016/j.jadohealth.2013.12.023.
Publichealth.columbia.edu. 2022. Abstinence Only Education is a Failure | Columbia Public Health. [online] Available at: <https://www.publichealth.columbia.edu/public-health-now/news/abstinence-only-education-failure> [Accessed 7 May 2022].
Scholars Strategy Network. 2022. Why Sex Education in the United States Needs an Update and How to Do It. [online] Available at: <https://scholars.org/contribution/why-sex-education-united-states-needs-update-and-how-do-it> [Accessed 8 May 2022].
SIECUS. 2022. California State Profile – SIECUS. [online] Available at: <https://siecus.org/state_profile/california-state-profile/> [Accessed 7 May 2022].
SIECUS. 2022. Louisiana State Profile – SIECUS. [online] Available at: <https://siecus.org/state_profile/louisiana-state-profile/> [Accessed 7 May 2022].
USC-MSN. 2022. America’s Sex Education: How We Are Failing Our Students. [online] Available at: <https://nursing.usc.edu/blog/americas-sex-education/#:~:text=Research%20published%20by%20the%20Journal,sexually%20transmitted%20diseases%20and%20infections> [Accessed 7 May 2022].
Guttmacher Institute. 2022. Sex and HIV Education. [online] Available at: <https://www.guttmacher.org/state-policy/explore/sex-and-hiv-education?gclid=Cj0KCQjw37iTBhCWARIsACBt1IwFAJ3xBLUBZquVelUKX69Bd67AA71HgrhZmlYB4_J2660wZjsz6GIaAptGEALw_wcB> [Accessed 7 May 2022].
 NOLAbeings
Multimedia artist Claire Bangser created NOLAbeings as a portrait-based story project that marries...
NOLAbeings
Multimedia artist Claire Bangser created NOLAbeings as a portrait-based story project that marries...
 Data corner: Adobe Suite (create a PDF, social media graphic, presentation, edit a photo and video
Data corner is where you go to work with analytics and top tech skills. It takes on everything from PERL and SQL to Canva and Sprout Social.
Data corner: Adobe Suite (create a PDF, social media graphic, presentation, edit a photo and video
Data corner is where you go to work with analytics and top tech skills. It takes on everything from PERL and SQL to Canva and Sprout Social.

Power washing is a great way to extend the lifespan of industrial roofing systems. By avoiding the buildup of moss, algae, and dust, commercial roofs are kept in good shape, decreasing the necessity for pricey restorations and replacements. Algae and algae can hold water, resulting in roof damage and leaks. Consistent pressure cleaning removes these harmful elements, safeguarding the roofing material and structure. Furthermore, a neat roofing system reflects more light, reducing heat absorption and decreasing energy bills. By ensuring a tidy and intact roof, commercial property owners will increase its lifespan and protect their investment. If you’re curious, please visit my residential and commercial pressure cleaning services website to discover more.
Roof Soft-Washing near Rancho Cordova for Chevron
Improving Solar Performance f8192d2